10 Reasons Not to Have Bariatric Surgery (and Safer Alternatives)
Thinking about weight loss surgery? Learn key reasons to pause, the real risks, and non-surgical options like ESG that can support lasting weight loss.
Everself Team
Team @ Everself
Every few weeks, someone considering weight loss surgery asks: “Should I go for bariatric surgery?” Spend a few minutes researching, and you’ll see two extremes—before-and-after transformations on one side, and people talking about complications, strict diets, and long-term adjustments on the other
Bariatric surgery works. That’s not the debate. It leads to significant weight loss and can improve serious health conditions.
What often gets missed is everything that comes with it such as surgery, recovery, risks, lifelong supplements, and the fact that most procedures can’t be undone.
This guide outlines the key reasons not to have bariatric surgery, so you can understand the risks, long-term trade-offs, and whether surgery is the right step for you right now. It also covers non-surgical weight loss procedures such as ESG and gastric balloons, which offer meaningful weight loss with lower risk and shorter recovery times, so you can decide what fits your life before committing.
Why Bariatric Surgery Helps Some People
Bariatric procedures such as gastric bypass and other surgical approaches have strong clinical evidence behind them. One of the most important long-term studies in this area is the Swedish Obese Subjects (SOS) trial, a large prospective controlled study that followed patients for up to 20 years.
Compared with people receiving usual care, those who underwent bariatric surgery experienced significantly greater long-term weight loss and lower risks of conditions such as diabetes, heart attack, stroke, and overall mortality.
Long-term follow-up from the SOS study showed that patients maintained substantial weight loss for decades, with average reductions of about 23% at 2 years and roughly 18% at 20 years. These findings highlight why bariatric surgery remains an effective treatment option for people with severe obesity and obesity-related health conditions.
Non-Surgical Alternatives You Can Explore First
Before any surgical conversation, it’s worth understanding what’s available on the non-surgical side, especially when comparing bariatric surgery vs non-surgical options.
ESG Stomach Tightening® is Everself’s flagship one-time, non-surgical endoscopic procedure. It uses sutures placed through the mouth to reduce stomach size from the inside. Most patients return home the same day and resume normal activities within two to three days.
ESG is often positioned as a middle ground, and understanding the ESG weight loss pros and cons helps set realistic expectations before choosing it.
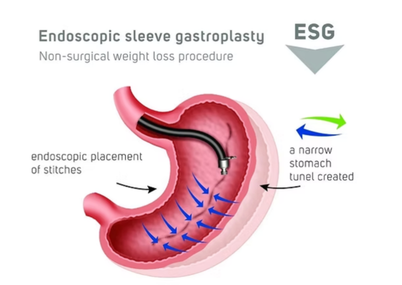
Caption: ESG reduces stomach size using internal sutures without surgery
Alt text: Endoscopic sleeve gastroplasty diagram showing sutures creating a smaller stomach for weight loss
Source: https://www.amgimed.com/esg-procedure
Average outcomes are around 20% total weight loss, supported by The Everself Program: 12 months of concierge care from a multidisciplinary team.
The gastric balloon is another option. It is a reversible, non-surgical procedure that is removed after six months. It helps patients feel full sooner. It’s a strong fit for people who want a jump-start or aren’t ready for a longer-term procedure, with average TWL gains of 10–15%.
-
Bariatric Surgery Is Still Major, Irreversible Surgery
Most bariatric procedures permanently change your anatomy. That’s the baseline.
In a sleeve gastrectomy, about 75–80% of the stomach is removed. In a gastric bypass, the stomach is reduced and the intestines are rerouted. These are structural changes that cannot be reversed.
If complications occur or outcomes fall short, options are limited. Revision surgeries are possible, but they are more complex, carry a higher risk, and are not guaranteed to fix the issue.
For patients with severe obesity and serious health conditions, this level of intervention can be justified. But if your BMI is lower, your health risks are moderate, or you’re not fully comfortable with permanent changes, this becomes one of the key reasons to avoid bariatric surgery and explore less invasive paths first.
-
Understanding Short- and Long-Term Risks
Bariatric surgery carries real short-term risks: bleeding, anastomotic leaks, blood clots, and infection. These are uncommon in experienced centers, but they’re not zero. Longer-term complications can include:
- Dumping syndrome: Rapid gastric emptying that can cause nausea, dizziness, diarrhea, fatigue, and low blood sugar after meals. Reported in up to ~40% of patients after gastric surgery, especially after bypass and sleeve procedures
- GERD and acid reflux: Can develop or worsen after sleeve gastrectomy. Research suggests that around 20% of patients may experience GERD following sleeve surgery, requiring ongoing dietary management or medication
- Nutritional deficiencies: Especially B12, iron, calcium, and vitamin D, requiring lifelong supplementation
- Bowel obstruction: A less common but serious risk requiring medical attention
- Weight regain: A possible when habits shift or the stomach pouch expands over time
These are part of the broader risks and complications of bariatric surgery, including several bariatric surgery side effects long term that patients need to plan for. None of this is meant to frighten you. It’s meant to ensure you go into any decision with the full picture.
-
Weight Loss Is Not Guaranteed Forever
Bariatric surgery can lead to significant weight loss, especially in the first 1–2 years. But those results don’t automatically last.
Over time, some patients begin to regain weight. This can happen gradually as habits shift, hunger signals change, or the body adapts metabolically. In some cases, the stomach pouch may also stretch slightly, allowing larger portions over time.
Long-term studies show that weight regain is not unusual. Research published in The New England Journal of Medicine found that approximately one-third of patients regain a significant portion of their lost weight within 10 years, and around one-third regain most or nearly all of the weight they initially lost.
That’s why bariatric surgery is best seen as a tool that requires ongoing management, not a one-time fix.
-
Lifelong Nutrition and Supplement Needs
After gastric sleeve or bypass surgery, your digestive system absorbs nutrients differently, sometimes significantly less efficiently. This means lifelong supplementation of vitamins and minerals is medically required.
For many patients, this is an acceptable trade-off. For others, the idea of daily supplements, regular lab work, and careful attention to nutrient intake indefinitely is a meaningful lifestyle shift worth weighing carefully before surgery.
With ESG, the stomach is reshaped but not removed. Nutrient absorption pathways remain intact, which means the supplementation burden is substantially lower.
-
Recovery Time, Work, and Family Life
Bariatric surgery typically requires a one-to-three-day hospital stay, followed by two to six weeks of limited activity. Driving, heavy lifting, and returning to full work capacity all take time. For people managing caregiving responsibilities, demanding jobs, or limited support at home, this timeline is a real consideration.
ESG, by contrast, is an outpatient procedure. Most patients go home the same day and return to normal activities within two to three days.
Planning recovery realistically
Ask yourself: Do I have adequate support at home? Can I take the necessary time off work? Who handles caregiving responsibilities during recovery? This would help you decide the type of surgery you would want to commit to.
-
Are You Ready for Long-Term Lifestyle Changes?
Surgery works best alongside sustained behavioral change. Smaller portions, mindful eating, consistent movement, and regular follow-up are important after bariatric surgery. Patients who don’t have strong lifestyle habits in place before surgery often struggle more in the years that follow.
If you’re not yet confident in your readiness for those changes, that’s important information. For many people, this becomes one of the practical reasons not to have bariatric surgery yet, and instead focus on building sustainable habits first.
-
Emotional Health and Relationship With Food
For many people, the relationship with food is layered with emotion such as stress eating, binge patterns, using food to cope with anxiety or difficult experiences. Surgery changes the physical capacity of the stomach. It doesn’t address the emotional dimensions of eating.
Patients who enter surgery without support for emotional eating patterns are more likely to experience psychological challenges afterward, including frustration, disappointment, and in some cases, transferring eating behaviors to other habits. This does require proactive attention.
If this resonates, consider pairing any weight loss intervention with professional behavioral support.
-
Do You Clearly Meet Surgical Criteria?
Most bariatric surgeons follow evidence-based eligibility guidelines: a BMI of 40 or higher, or a BMI of 35 or higher with a qualifying health condition.If you’re below these thresholds, many surgical programs won’t accept you as a candidate, which also answers a common question around who should not have bariatric surgery.
ESG Stomach Tightening® is approved for patients with a BMI of 30 or higher, and may also be appropriate for patients with a BMI of 27–29.9 with an obesity-related condition. This makes it accessible to a meaningfully broader group of people.
What to do if you don’t meet surgical criteria
An endobariatric specialist can help you understand which options are clinically appropriate for your profile, and map out a care plan that fits your body and your goals without defaulting to “wait until your BMI is higher.”
-
If You Prefer Less Invasive, Scar-Free Options
Some patients feel strongly that they want to avoid external scars or an extended hospital stay. That’s a legitimate preference.
For many people, the appeal comes down to the benefits of non-surgical weight loss procedures like lower risk, faster recovery, and more flexibility over time.
Alternatives to traditional bariatric surgery like ESG and the gastric balloon are performed entirely through the mouth. No incisions or stitches. No surgical team in a hospital OR. For patients who have been told surgery is their only real option, this is often the piece of information they were missing.
-
When Bariatric Surgery May Still Be the Right Choice
For some patients, particularly those with severe obesity, a BMI significantly above 40, and multiple serious health conditions, bariatric surgery at an experienced, high-volume center may genuinely offer the greatest long-term health benefit. The evidence supporting surgery in this population is strong.
The goal is to find the right level of intervention for your body, your health, and your life stage. If surgery is the right answer for you, a thoughtful specialist will help you see that clearly.
And if non-surgical weight loss might be a better fit than surgery applies to your situation, the same specialist will be honest about that too.
How to Decide Your Next Step
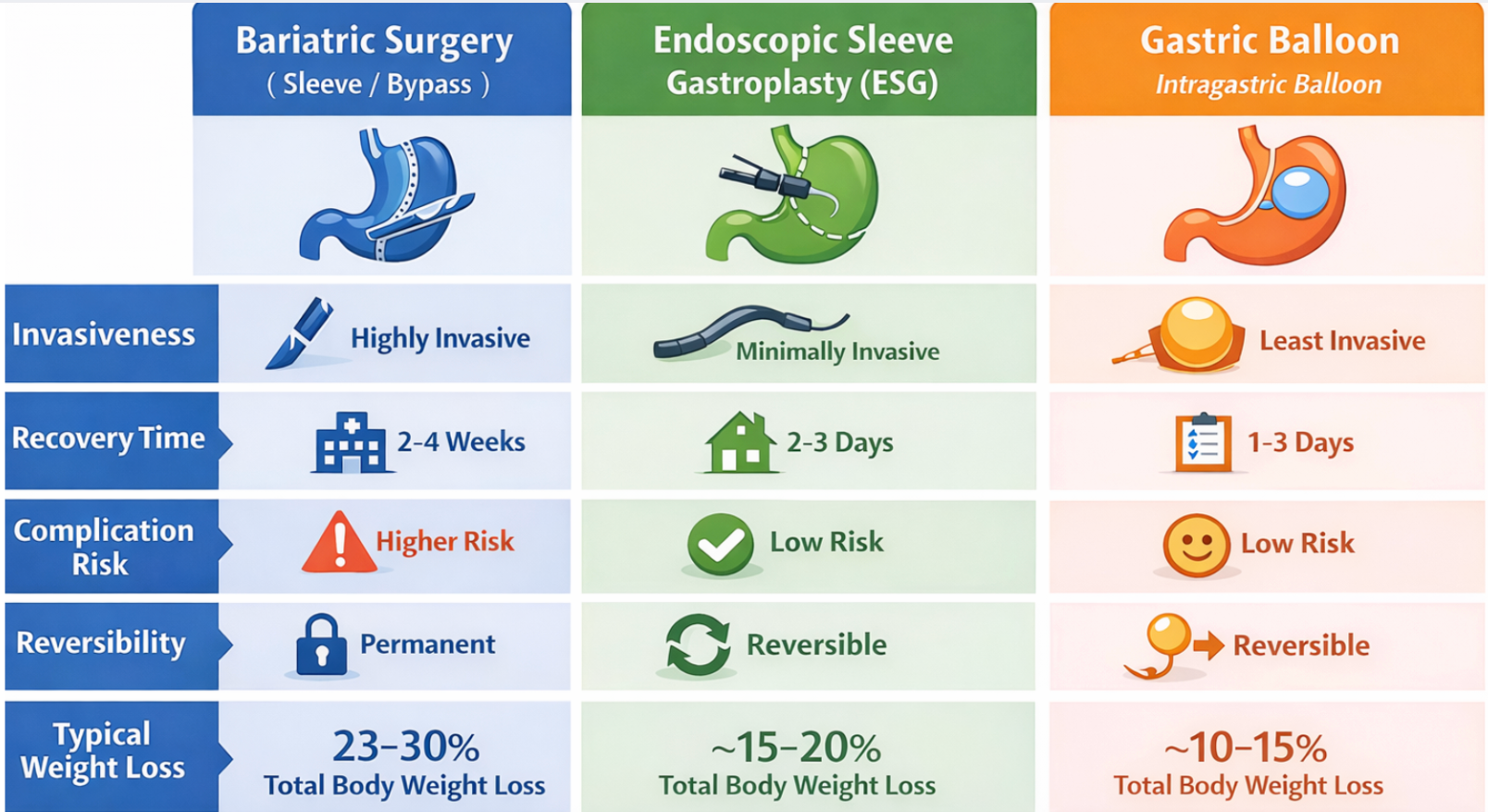
Caption: Bariatric surgery vs ESG vs gastric balloon: key differences at a glance
Alt text: Comparison chart of bariatric surgery, ESG, and gastric balloon across risks, recovery, reversibility, and weight loss.
If you’ve read this far, you’re doing exactly what an informed patient does: gathering the full picture before committing. You’ve also seen the key reasons not to have bariatric surgery, and how those trade-offs might apply to your own situation. So, here are some practical steps to take next.
- Write down your personal priorities and concerns. What matters most is recovery time, reversibility, weight loss outcomes, and ongoing support? Putting it in writing helps you ask better questions in any consultation.
- Talk with an endobariatric specialist about both paths. The right specialist will walk you through surgical and non-surgical options side by side, explain what realistically fits your profile, and help you avoid jumping into something that doesn’t align with your goals.
If you want that kind of clarity, you can speak with our team. We’ll help you understand your options, without pressure, and map out a plan that actually fits your body and your life.